Will artificial intelligence revolutionize the medical profession?
Coined in the 1950s, the term “artificial intelligence” (AI) refers to a computer system capable of reasoning, learning, and planning, with behavior reminiscent of that of intelligent biological systems. Machine learning relies on programming that is not solely determined by code but also adapts to the data it is fed.
Matthias Brunn, University of Montpellier and William Genieys, Sciences Po – USPC
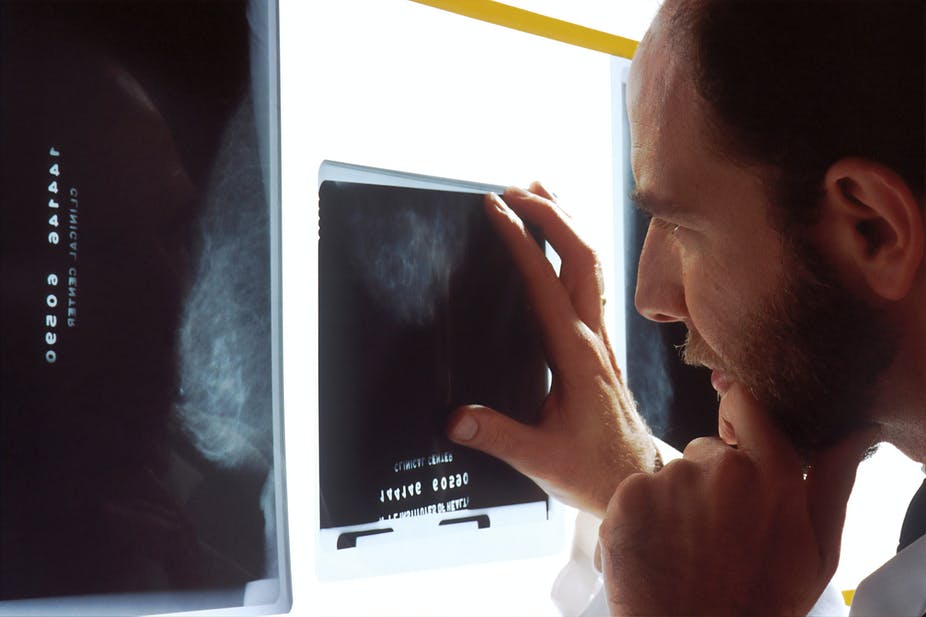
National Cancer Institute – Unsplash, CC BY
For example, in the formal context of artificial neural networks, mathematical algorithms use an iterative process to determine the best way to represent the relationship between multiple variables. Each neuron represents a relatively simple function, which makes it possible to construct highly complex functions within a large network.
Medicine, for its part, is a long-standing and widely respected institution in our societies, as evidenced by the trust placed in healthcare professionals during the COVID-19 pandemic. And we tend to view it as a great ship whose stability cannot be threatened.
Yet the reality is quite different. In the coming decades, medicine is likely to undergo a profound transformation driven by AI— a true “revolution,” in the words of President Emmanuel Macron. And to grasp the scale of these coming changes, one need only look at the Health Data Hub, a platform launched by the French government in November 2019 that allows researchers to use data from the national healthcare system to train artificial intelligence models.
Some 10 research projects have already been selected to make use of this platform. And all aim to improve the effectiveness of medicine. For example, “Deepsarc” aims to identify the best treatment regimens for sarcoma, “PIMPON” seeks to help prescribers better understand dangerous drug interactions, “Hydro” seeks to predict heart failure episodes in patients with pacemakers, “Oscour” aims to leverage emergency department data to improve public health surveillance, and “Deep.Piste” will evaluate the contribution of artificial intelligence to organized breast cancer screening—a significant contribution according to a study published last January in Nature and conducted among six radiologists.
While the medical profession has always been able to capitalize on technological innovations (X-rays, MRIs, etc.), it now finds itself facing an unprecedented paradigm shift. Will algorithms come to replace healthcare professionals? In which fields will the battles be fought?
A constantly changing world
According to American sociologists Rue Bûcher and Anselm Strauss, any profession can be defined as a world composed of segments, each with different conceptions of professional practice and varied identities that transform, persist, develop, and/or disappear. Various medical disciplines thus find themselves in competition with one another. For example, when it comes to the management of severe coronary artery disease, there may be a conflict between cardiologists who favor angioplasty and stent placement, and cardiac surgeons who instead advocate for open-heart bypass surgery.
Overall, with state support and in competition with other groups such as spiritual healers, the medical profession secured a monopoly on the provision of healthcare inthe 20thcentury. To achieve this, it relied on a coherent and scientific system aimed at defining, classifying, and diagnosing somatic and/or psychological ailments. But it was also its ability to self-organize (into disciplines, learned societies, unions, etc.) that conferred upon medicine its authority in matters of health.

: Nina Aldin Thune, CC BY-SA
In this context, AI can be seen as a new technical innovation capable of assisting doctors, but also of strengthening their position relative to other disciplines. Yet within this highly hierarchical profession, technological choices are made by elites who operate according to a “mandarin” logic, based on a mix of conservative professional values and a rejection of the state’s bureaucratic power. Even though, for each discipline, the decision to use AI depends on a comparative assessment of its benefits and risks, based on past experience.
As a result, psychiatrists tend to be skeptical that AI can perform the complex tasks of their daily work, as psychiatry is generally less tech-savvy than other disciplines. Conversely, medical imaging is a field where AI’s performance is already rendering certain radiologist roles obsolete. In fact, we are witnessing the emergence of a first generation of radiology professors who have built their careers on the use of AI in medical imaging.
Significant disruptive potential
By going beyond the scope of traditional technical innovations, AI is bringing about a true revolution for medical professionals. The reasons are primarily technical: in addition to unprecedented speed in performing certain tasks, it enables the development of autonomous learning—as evidenced by the rapid advances in instant language translation, now available for free online with major implications for the job market. But the revolution also stems from the anthropomorphic aspect of AI…
Artificial neural networks, humanoid robots, and chatbots are prime examples of this. These digital conversational agents use text- and/or voice-based AI methods to mimic human behavior through adaptive dialogue. They are seen as a means of providing mental health care in regions where such services are scarce, or for people who have difficulty expressing their feelings to another human being. In short, AI is becoming a social actor in its own right (or an “actant” in Bruno Latour’s framework), which increases its disruptive potential.
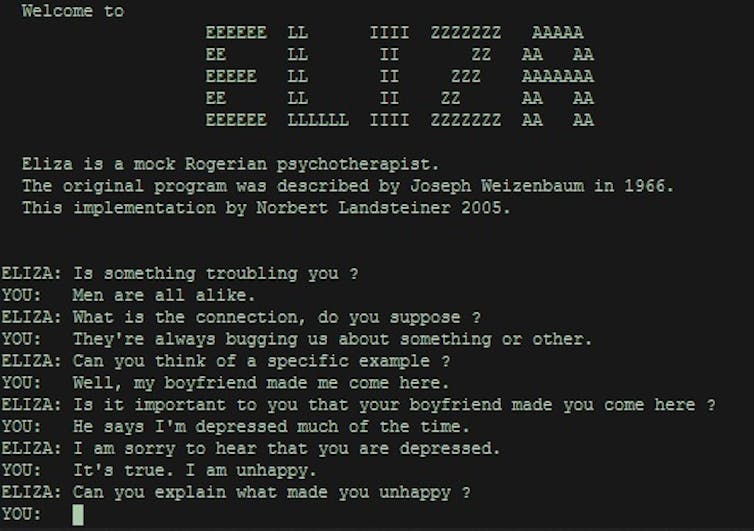
Wikipedia
These two aspects of AI go hand in hand and are likely to profoundly transform the world of medicine by upending the established order. As a result, radiology could become a specialty with fewer positions and a profile that is more “clinical” than “diagnostic.” Conversely, psychiatry, which currently attracts few students, is likely to see its profile strengthened due to its social dimension, which is difficult to replace with AI applications.
In fact, it is precisely by drawing on this aspect and its fundamental principles—empathy, the intimacy of the patient-practitioner relationship, and medical confidentiality—that the medical profession as a whole could redefine its profile and scope of practice. For when it comes to healthcare, various actors outside the medical world have indeed positioned themselves to address somatic and/or psychological distress through AI: this is notably the case with
Tech giants like Google, which funds research on AI in healthcare; Facebook, which uses AI to detect suicide risk among its users; and Microsoft, which hosts the Health Data Hub in France.
Just as a container ship—though accustomed to storms—can be battered by a barrage of rogue waves, the medical profession is now facing an unprecedented situation. And even though it has the resources needed to navigate these waters, the force of the elements may force it to chart a new course. Whatever the outcome, the transformation will be profound.![]()
Matthias Brunn, Political Science Researcher at CEPEL/CNRS, University of Montpellier and William Genieys, CNRS Research Director at the CEE at Sciences Po, Sciences Po – USPC
This article is republished from The Conversation under a Creative Commons license. Readthe original article.