"Exotic" viruses in France: a topic that is more relevant than ever
The Usutu virus, the Zika virus, the chikungunya virus, and the dengue virus… In recent years, these exotic-sounding names have all made their way into the French media. And for good reason: responsible for diseases that until now were confined to remote regions, these viruses are breaking out of the areas where they have long been endemic and setting out to conquer our planet. France is not immune to this threat, neither in its overseas territories nor in its metropolitan regions, as evidenced by the ongoing spread of the dengue and Usutu viruses around the Mediterranean basin. Which viruses should we be watching? What is the current situation? Here is what we have learned in recent years from the work of the surveillance networks currently in place and the research laboratories studying these viruses.
Yannick Simonin, University of Montpellier

Diseases transmitted from animals to humans
Many emerging infectious diseases are transmitted to humans by an animal “vector,” often a blood-sucking arthropod such as mosquitoes, culicoid midges, sandflies, or ticks.
In such cases, if the disease is caused by a virus, it is referred to as an “arbovirus,” and the virus involved is described as an “arbovirus” (from the English “arthropod-borne virus”). Since 2015, the World Health Organization (WHO) has compiled an annual list of priority diseases. Updated in 2021, this list includes only viral diseases. Of the nine listed, three are arboviruses: Zika virus disease, Crimean-Congo hemorrhagic fever, and Rift Valley fever.
It is also important to note that most arboviral diseases are zoonoses. In other words, they originate in domestic or wild animals that carry the pathogen. The pathogen is then transmitted to humans when they are bitten by a vector arthropod that has previously fed on the blood of an infected animal.
What happens next depends largely on the specific arbovirus involved. Some can be transmitted from one person to another, always via a vector. Others may also spread through additional transmission routes (the Zika virus, for example, can be transmitted by mosquitoes and through sexual contact). It also happens that certain arboviruses do not spread between humans: in such cases, humans are said to be an “epidemiological dead end.” This is the case, for example, with the West Nile virus or the Rift Valley virus.
Among the main vectors of arbovirus transmission are mosquitoes, particularly the Asian tiger mosquito (Aedes albopictus). Having recently invaded our region, it has quickly established itself here. Indeed, this species alone is capable of transmitting several “exotic” viruses.
[Nearly 70,000 readers rely on The Conversation’s newsletter to better understand the world’s major issues. Subscribe today]
The tiger mosquito continues its rapid spread
Driven by international trade, the spread of the tiger mosquito (Aedes albopictus)—a vector for several “exotic” viruses—has been remarkably rapid.
Native to Asia, this small black mosquito with a white-striped body and legs was first detected in southern France in 2004, in Menton. Less than twenty years later, it is present in 67 of the 96 metropolitan departments (up from 58 in 2020). In the coming years, the expansion of its range will be unstoppable.
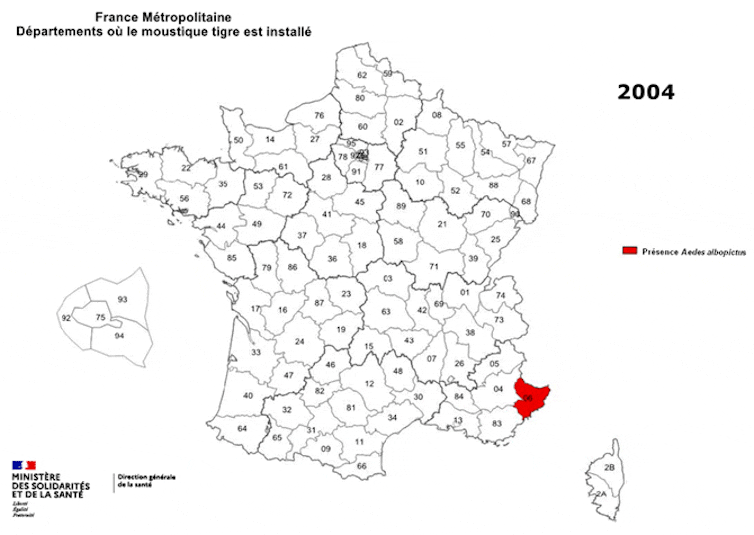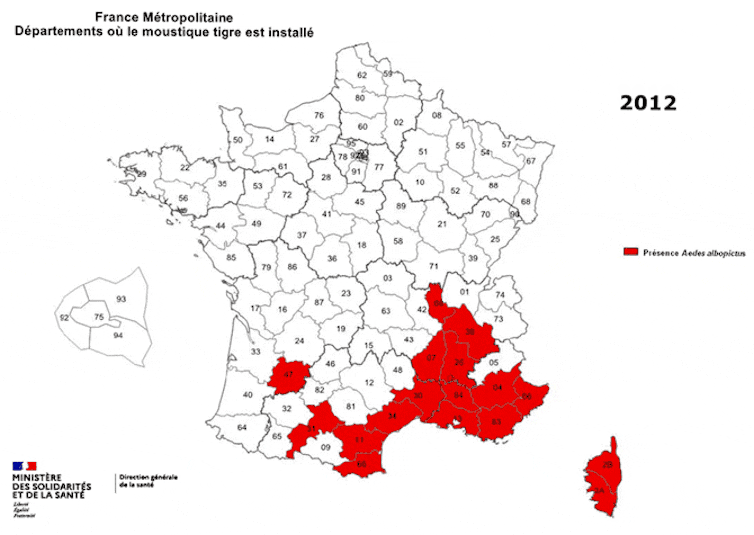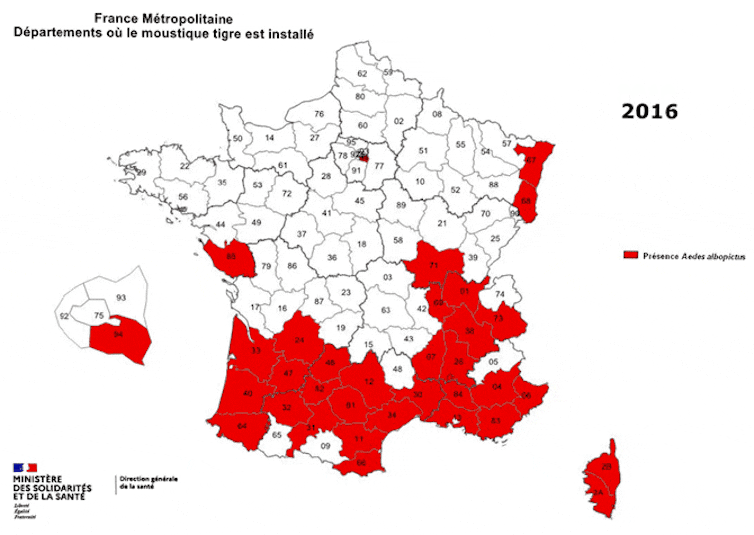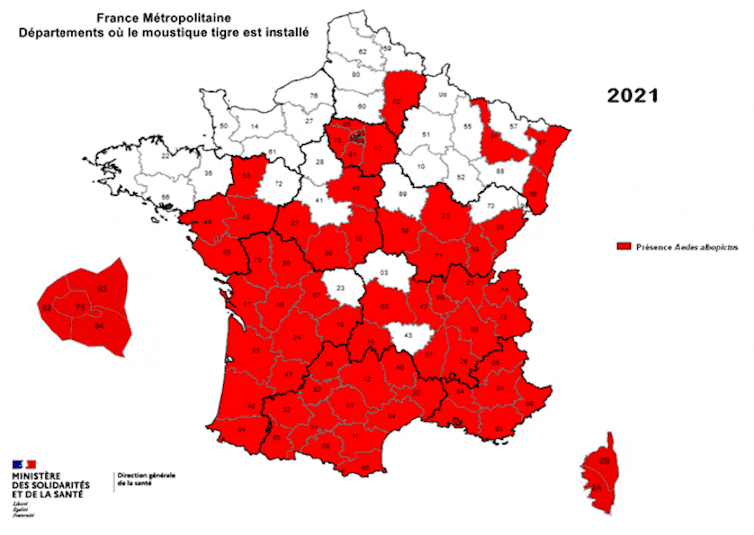
Ministry of Solidarity and Health – Directorate General for Health
One of the distinctive features of this mosquito is its ability to transmit various viruses that cause diseases, the best known of which are probably the Zika virus, the chikungunya virus, and the dengue virus.
Dengue Fever: An Uptrend in Local Cases
The dengue virus appears to have found a favorable environment in the southern regions of our country. Indeed, while the number of dengue cases remains low in mainland France—estimated at fewer than thirty in recent years—the upward trend is nevertheless confirmed.
This is evidenced by the rise in so-called “autochthonous” cases, meaning that the disease was contracted within France, as opposed to imported infections, which are diagnosed in France but were contracted abroad during travel. The departments in southern and southeastern France, such as Hérault, Gard, Var, and Alpes-Maritimes, are most at risk of the disease, particularly due to the combination of a high density of tiger mosquitoes and heavily urbanized areas.

Wikimedia Commons / Centers for Disease Control and Prevention
Given that dengue fever is largely asymptomatic (in 50% to 90% of cases, depending on the outbreak), and that in symptomatic individuals, the symptoms of the disease (fever, headache, muscle aches, etc.) can easily be confused with those of the flu or, more recently, COVID-19, the number of cases is certainly greatly underestimated.
Although the illness it causes is usually mild, the dengue virus can nevertheless lead to a potentially fatal form in about 1% of cases: so-called “hemorrhagic” dengue, as it is accompanied by bleeding in multiple organs. In addition, certain neurological complications have also been reported.
Chikungunya is keeping a low profile
First identified in Tanzania in 1952, the chikungunya virus has been circulating for several decades in Africa, India, and Asia, as well as in the Indian Ocean. In fact, it was the outbreak that struck Réunion, Mauritius, Mayotte, and the Seychelles in 2005 that helped bring it to the attention of the French public.
"The 'bent man's disease'" (a possible translation of "chikungunya," a term derived from Makonde, a Bantu language spoken in Tanzania) is characterized in particular by the onset of fever and severe joint pain. These symptoms are highly debilitating and often affect the hands, wrists, ankles, or feet. Headaches and muscle pain, as well as bleeding from the gums or nose, have been frequently reported. Recovery can take several weeks, and the pain may sometimes persist for several years.
The first two locally acquired cases of chikungunya were detected in France in 2010, in the Var department. Since then, about 30 locally acquired cases have been reported, including two major outbreaks: one in the city of Montpellier in 2014 (11 confirmed cases and 1 probable case) and the second in the Var region in 2017, with 17 cases reported.
The chikungunya virus has been relatively quiet in France in recent years, with three imported cases in 2021 and five so far this year, according to figures from Santé publique France. However, the virus remains under close surveillance, particularly because its spread by the tiger mosquito in temperate European regions cannot be ruled out.
In anticipation of a resurgence of the Zika virus
The Zika virus, meanwhile, made headlines in 2015–2016. It caused a massive outbreak, primarily in Latin America. More than one million people were infected. The most serious complication associated with this virus is the development of microcephaly (a reduced head circumference in the fetus) in infected pregnant women.
In France, two locally acquired cases were identified in 2019 in the Var department, although the transmission chains—particularly those involving vectors—could not be clearly established.
Although it remains on the World Health Organization’s list of the 10 most dangerous diseases, this virus has, however, mysteriously all but disappeared from the public eye in recent years. Its return to the forefront of the viral scene is, however, far from out of the question: it has recently made headlines again in Thailand, and five travelers have contracted the disease in Germany, the United Kingdom, and Israel after visiting this Southeast Asian country.
Although little is known about the mechanisms underlying the emergence of the Zika virus, seroprevalence studies (measuring the presence of antibodies in the blood) show that it is still actively circulating in certain regions (particularly on the African continent).
Monitoring this requires particular vigilance on the part of the scientific community, in order to prepare for a potential resurgence.
Good old Culex isn't left out either
One of our “common” mosquitoes, Culex pipiens, found throughout France, is also capable of transmitting “exotic” viruses to us. This is particularly true of the West Nile and Usutu viruses, two closely related viruses that can occasionally cause severe neurological disorders such as encephalitis (inflammation of the brain), meningitis (inflammation of the meninges), or meningoencephalitis (inflammation of the meninges and the brain) in humans.
A study conducted by our team and published in 2022, in collaboration with ANSES and CIRAD, showed that these two viruses are becoming established on a long-term basis in certain areas of our country, particularly in the greater Camargue region. Indeed, they are regularly found not only in human blood samples, but also in animals such as birds (their natural reservoirs), dogs, horses, and mosquitoes.
So far, their impact on human health remains limited: only one case of Usutu virus infection has been identified in France to date, in Montpellier, while about thirty cases of West Nile virus have been reported over the past five years. It is nevertheless important to monitor the spread of these viruses, as several strains with varying degrees of virulence are currently circulating, which calls for caution. This is all the more important given that a major outbreak struck Europe in 2018, with more than 2,000 cases identified and over 180 deaths reported.
In addition, Italy—like other countries in southern Europe—has reported an early outbreak of West Nile virus this year, with nearly 150 cases identified by mid-August, indicating that the virus is becoming increasingly established in the southern part of the continent.
Human Activities and Emergencies
The transmission of a disease from animals to humans does not necessarily lead to an outbreak, a large-scale epidemic, a pandemic, or the spread of the disease to new areas. Such events are, in fact, the result of a combination of many factors.
The problem is that trade and tourism, which are growing exponentially in our hyperconnected world, can facilitate the spread of certain vectors and thus increase the risk of disease transmission.
This risk is further exacerbated by environmental and climate changes. Weather conditions—particularly temperature, humidity, and precipitation—affect the geographic distribution, activity, reproduction rates, and survival of these vectors, especially mosquitoes. Furthermore, climate change and human impact on the environment sometimes influence animal behavior, for example by altering the range of certain species, which can increase interactions between animals and humans.
Such environmental changes have led to outbreaks of Argentine hemorrhagic fever, caused by the Junin virus. In the 1950s, to intensify corn cultivation, massive land clearing was carried out, notably through the use of herbicides. This environmental change led to a proliferation of rodents, some of which were carriers of the virus, causing the disease to reach epidemic proportions, particularly among agricultural workers. Thousands of people were subsequently infected. A similar situation was also observed in East Asia during the conversion of land for rice cultivation, with the Hantaan virus responsible for “Korean hemorrhagic fever.”
Other factors contributing to the emergence of new diseases include, in particular, socioeconomic factors such as the increase in the movement of goods and people—especially through intercontinental air travel—and the ever-growing expansion of urban areas. High population densities, which facilitate the rapid spread of diseases, as well as water supply challenges linked to rapid urbanization, contribute in particular to the proliferation of mosquitoes that may carry viruses.
As evidence of the importance of these factors, during the COVID-19 pandemic, the number of imported “exotic” infections (i.e., those contracted while traveling) dropped significantly, mainly due to the sharp decline in international air travel. With the marked recovery of air travel, however, an increase in such cases is expected this year.
This situation could lead to outbreaks of cases in France, as an infected person arriving in the country could in turn transmit the disease to others, particularly if the vectors responsible for transmitting the disease are present.
Prevention: The Best Defense Against "Exotic" Viruses
In the absence of an effective antiviral drug or vaccine—as is the case with chikungunya or Zika—or when the vaccine has certain limitations (as is the case with dengue, where the only currently approved vaccine has the drawback of increasing the risk of hospitalization and severe dengue in people who have not previously been infected with the dengue virus), the only solution is to anticipate the emergence of these pathogens.
The best way to achieve this is to establish appropriate and responsive networks that operate at the local level, in order to effectively study the interactions between animals, humans, and their various environments, using an approach known as One Health (covering both human and environmental health).
Since the onset of the COVID-19 pandemic, national and international viral disease surveillance networks have expanded. Unfortunately, their capabilities remain far below what is needed to effectively monitor the circulation of high-risk viruses, not only in endemic countries but also in countries where these viruses are emerging.
The emergence and subsequent rapid spread in 2020 of the SARS-CoV-2 coronavirus, which caused the COVID-19 pandemic, has had a major impact on our health, our behaviors, and our daily lives. This situation has brought home to us just how important it is to monitor and study “new” viruses.
But beyond these previously “unknown” viruses, it is also essential to focus on “neglected” viruses, as they cause diseases that are rampant far from our borders.
The spread outside the African continent, and particularly in Europe, of the Monkeypox, the virus responsible for [monkeypox], is a good example of the challenges associated with such surveillance…![]()
Yannick Simonin, virologist and associate professor of surveillance and research on emerging diseases, University of Montpellier
This article is republished from The Conversation under a Creative Commons license. Readthe original article.