To combat back pain, simply moving more isn't enough
“Back pain? The best treatment is movement.”The slogan has been featured heavily on television and billboards for the past two weeks. The Health Insurance Agency has launched its first national campaign to encourage people suffering from lower back pain to engage in physical activity.
Gregory Ninot, University of Montpellier
Shutterstock
The goal of this campaign, which runs through December 18, is to challenge the common misconception that staying in bed is the best way to recover from a back sprain. While getting more exercise is certainly beneficial, is it really that simple?
Back pain affects about 1 in 10 people. This persistent pain in the lumbar vertebrae, located just above the tailbone, is known as benign or nonspecific low back pain. It leads to limited mobility, a more sedentary lifestyle, recurring negative thoughts, emotional difficulties, and repeated absences from work, as established by a study published in 2010.
Some people feel helpless; nearly 60% of those suffering from lower back pain thinking they wouldn't be able to recover. They resort to more and more treatments and care, without achieving any lasting benefit. And healthcare costs for the health insurance system are skyrocketing. For example, a French study of a cohort of patients seen by general practitioners showed that low back pain lasted longer than one year in 81% of patients, with an average total cost per patient over six months of 715 euros in 2007.
Out-of-pocket costs for patients are also rising, as Medicare covers only 35% to 70% of medical expenses, depending on the case.
Movement is necessary
To treat back pain, movement is essential, as the campaign. Taking the stairs instead of the elevator, getting off the subway or tram one stop early, biking whenever possible, and swimming are a good start. These physical activities are a necessary evil—far more effective than rest at relieving lower back pain.
Rest is a bad habit, one that people develop during occasional illnesses like the flu. By thinking that rest will cure lower back pain, we actually make it worse. The less people move, the less capable they feel of moving. Physical inactivity makes them more vulnerable to other health problems. Lower back pain worsens and becomes chronic. This process is known as the vicious cycle of deconditioning.
On the other hand, the danger lies in going too far, too fast, or too hard. Taking painkillers, overdoing exercise, or simply “putting up with it” (blaming aging, work-related stress, burnout, family pressures, and so on) may help you forget the pain, but it doesn’t solve anything.
Get more exercise, but not just any kind
Getting more exercise, yes, but not just any way. Research is increasingly exploring the rich field of non-pharmacological interventions. The French National Authority for Health (HAS),Inserm, and the French Academy of Medicine are all taking an interest in this area.
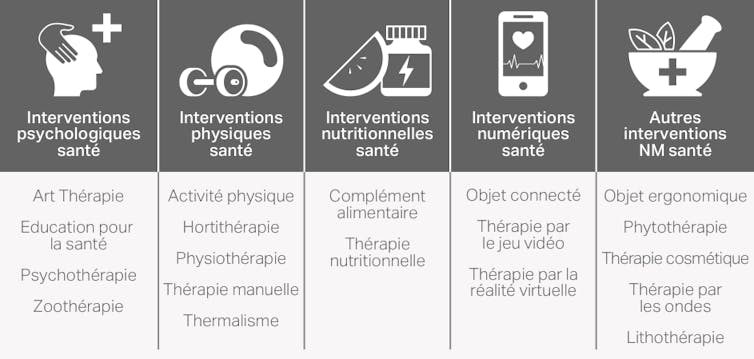
CEPS Platform, Universities of Montpellier
Non-pharmacological interventions (NPIs) specific to low back pain will target muscular aspects (such as strengthening postural muscles), neuromuscular aspects (such as flexibility), neurological aspects (such as pain management), postural aspects (such as workstation ergonomics), psychological aspects (such as pain desensitization and stress management), social aspects (such as work organization), and environmental aspects (such as bedding).
These NMTs will involve trained professionals, such as physical therapists, osteopaths, acupuncturists, adapted physical activity (APA) instructors, psychologists, or therapeutic education specialists.
Defining the dose, intensity, and frequency of these NMTs for each individual is essential to achieving satisfactory results.
Non-pharmacological interventions have been the subject of clinical studies evaluating their effectiveness in the treatment and prevention of low back pain. These include Pilates, Dru Yoga (a form of yoga practiced particularly in Great Britain), tai chi, adapted physical activity programs, osteopathy, chiropractic care, acupuncture, spa therapy, the Back School method (an “American back school” founded in 1969), the McKenzie method (originating in New Zealand in 1981), and finally, patient therapeutic education.

Antonika Chanel/Unsplash
An osteopathic treatment program specifically for lower back pain
Some studies are particularly noteworthy. For example, a clinical trial led by the team of British physician and researcher Nefyn Howard Williams evaluated the benefits of an osteopathic treatment method in people suffering from acute and subacute (i.e., mild) spinal pain. The randomized controlled trial included 201 participants aged 16 to 65. They had consulted their primary care physician for neck or back pain that had developed between 2 and 12 weeks prior.
Comparisons between the group receiving only standard care and the group undergoing 3 to 4 osteopathic sessions by a trained physician were conducted on three occasions: before the start of the intervention, at the end of the intervention (i.e., 2 months later), and six months after the intervention. The measurements focused on health status related to spinal pain, quality of life, the sensory and emotional dimensions of pain, and the cost-effectiveness of the care received.
The osteopathic sessions were spaced one to two weeks apart, within a maximum time interval of two months. The program included manual techniques and advice on regular physical activity. The results show, at the end of the two-month osteopathic intervention, a reduction in the intensity of spinal pain and an improvement in quality of life compared to the control group.
After six months, quality of life remained higher than in the control group. However, pain levels no longer differed between the two groups. Healthcare costs specific to spinal pain were significantly higher for the group receiving osteopathic intervention (88 euros per patient in total).
Psychotherapy tailored to lower back pain
Another study, this time involving psychotherapy. The trial, led by Swedish researcher Steven Linton’s team and published in 2015, evaluated the effectiveness of an intervention targeting workers and their employers to prevent work-related disability due to back pain. The intervention was compared to standard care for low back pain.
140 people aged 27 to 65 participated in this study, conducted at a Swedish health center. They suffered from low back pain and were at high risk of developing a chronic musculoskeletal disorder. For each person, the researchers recorded days lost from work due to musculoskeletal disorders, use of healthcare services, perceived health status, and pain intensity. Measurements were taken before and after the intervention, and then six months after the intervention.
Participants in the test group also received a brief psychological intervention based on the principles of cognitive-behavioral therapy (CBT). They participated in three face-to-face sessions with a clinical psychologist. Each session lasted between 60 and 90 minutes. The main objective of the intervention was to increase workers’ ability to manage the difficulties associated with their pain experience on their own in daily life, particularly in the workplace.
The study shows a halving of the average number of days of work absence six months after the intervention (38 days, instead of 17). The difference is statistically significant compared to the control group. The researchers also observed an improvement in perceived health status and a decrease in healthcare utilization for the test group. The intensity of pain experienced was reduced to the same extent in both groups.
Yoga: A Valuable Non-Pharmacological Intervention
Yoga is also one of the effective non-pharmacological treatments for low back pain. A meta-analysis published in January 2017 reviews all scientific studies on the use of yoga for low back pain and indicates its benefits. These yoga programs include physical exercises, breathing exercises, relaxation techniques, and meditation. They promote mindfulness and strengthen the connection between body and mind.
Who should you see to help manage back pain? The role of the primary care physician and/or specialist is to identify the cause of the pain, its severity, and its progression. They can then recommend the most appropriate non-pharmacological treatment for the patient’s lower back pain—or even suggest several options. These treatments may be used in conjunction with pain medication. This choice is based on the best balance between benefits and risks, as determined by scientific data, the doctor’s experience, the patient’s preference, and the feasibility of the treatment.
![]() General practitioners and specialists are becoming increasingly familiar with INMs and the local network of professionals who lead them. Some health insurance providers are beginning to cover certain ones. To combat back pain, you need to move more—but above all, move better.
General practitioners and specialists are becoming increasingly familiar with INMs and the local network of professionals who lead them. Some health insurance providers are beginning to cover certain ones. To combat back pain, you need to move more—but above all, move better.
Gregory Ninot, Professor of Health, Psychology, and Sports Science, University of Montpellier
The original version This article was published on The Conversation.