"Exotic" viruses in France: What do you need to know about chikungunya?
Since the start of summer, a record number of locally transmitted cases of chikungunya virus infection have been reported in France. Here’s what you need to know about this virus, which is spread by mosquitoes of the Aedes genus, such as the tiger mosquito ( Aedes albopictus).
Yannick Simonin, University of Montpellier
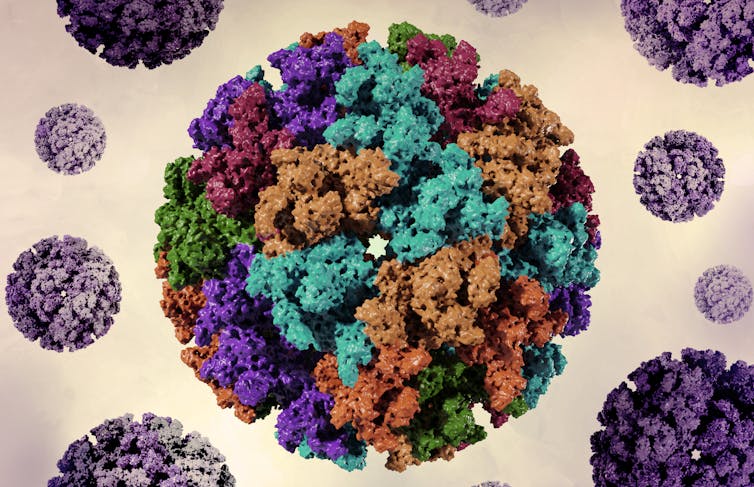
The chikungunya virus was first described in 1952 in Tanzania, on the Makonde Plateau. Its name derives from a word meaning “to become contorted” in the Kimakonde language, spoken primarily in southeastern Tanzania. It describes how the posture of patients, who are crippled by severe joint pain, changes during the course of the illness.
While most patients eventually make a full recovery, this virus is particularly dangerous for newborns and the elderly. In many cases, it can also lead to serious long-term effects, including joint pain and chronic fatigue. These symptoms can persist for several months or even years, significantly impairing the quality of life of those affected.
Biology and Transmission
The chikungunya virus (CHIKV) is an arbovirus, meaning a virus transmitted by arthropods. It is an enveloped virus with an RNA genome.
It is transmitted by female mosquitoes of various species belonging to the genus Aedes. TheAedes species most commonly responsible for its transmission are Aedes aegypti and Aedes albopictus, the infamous tiger mosquito. In rural areas of Africa, Aedes furcifer and Aedes africanus are also involved, along with several otherAedes species.
On the African continent, various animal reservoirs (primates, rodents, birds, etc.) have been identified as being involved in the virus’s cycle. The virus can therefore be transmitted from animals to humans, making it a zoonosis.
Livestock can also serve as a reservoir, but their role in transmission has not been clearly established.
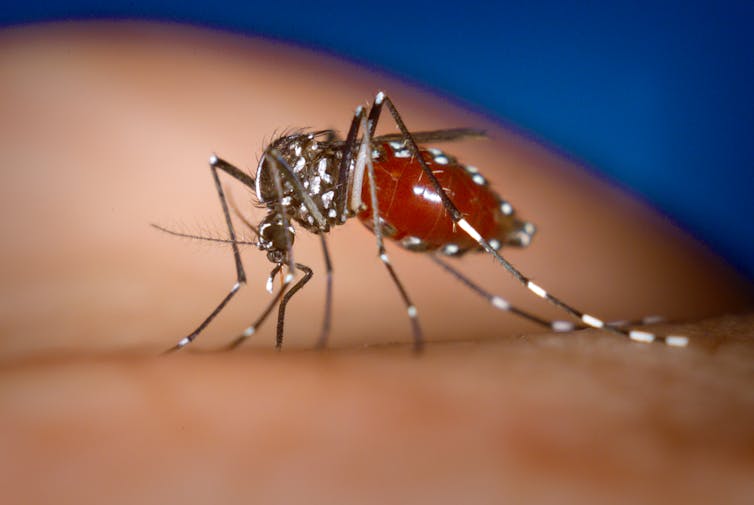
Although mosquitoes of the Aedes genus bite throughout the day, they are most active in the mid-morning and mid-afternoon. The risk of disease transmission is therefore highest during these times.
When a female mosquito feeds on a person whose blood contains the virus, the virus multiplies within the insect’s body over the course of about ten days, particularly in its digestive system and salivary glands. When the infected mosquito bites a new host, it systematically injects its saliva, primarily to prevent blood clotting and thus facilitate feeding. This is how it transmits the virus.
Once in the bloodstream of its new host, the virus multiplies again within a few days. Mosquitoes that bite the newly infected person will in turn become infected, continuing the cycle of viral transmission… This is how clusters of locally acquired cases—and even epidemics—emerge.
During outbreaks, it is therefore the transmission of the virus from one person to another that fuels the epidemic. A person carrying the virus can transmit it during the “viral shedding” phase (when the virus is present in the blood), which lasts from one to two days before symptoms appear and up to seven days afterward.
Infection can also occur through exposure to contaminated blood (throughtransfusion, a puncture with a contaminated needle, splashes, or contact, etc.). Furthermore, although rare, the virus can also be transmitted from mother to child during childbirth, with serious consequences for the newborn.
The chikungunya virus is highly fragile outside its host and does not survive well in the environment. Therefore, unlike many other viruses, it is not transmitted through contaminated objects or surfaces.
Symptoms
According to studies, infection with the virus is asymptomatic in only 5 to 40% of cases. The majority of infected individuals therefore develop symptoms, unlike with other mosquito-borne viruses such as dengue or Zika.
In people who develop symptoms, signs of the disease usually appear one to twelve days after being bitten by an infected mosquito (on average, two to three days).
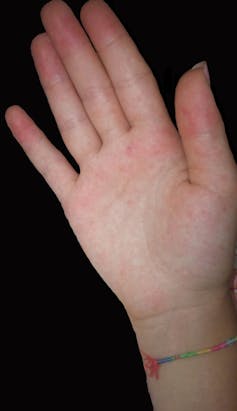
This fever is accompanied by joint pain, which is often severe and primarily affects the extremities (hands, feet, wrists, and ankles) as well as the knees, and more rarely the hips or shoulders. This pain is mainly due to inflammation resulting from the infection. Patients also often experience headaches and significant muscle pain (in 70% to 99% of cases), as well as a rash on the limbs and trunk.
Most patients make a full recovery. The fever usually subsides within two to seven days, the rash within two to three days, and joint pain within a few weeks.
However, in some people—particularly those over 40 or those with a history of joint disease—a chronic form of the disease may develop. In such cases, certain symptoms persist. Joint pain, in particular, can last for several years after the infection. This condition can be very debilitating in daily life, especially since it may be accompanied by chronic fatigue.
Some studies estimate that between 30% and 40% of symptomatic adult patients still experience persistent joint pain beyond three to six months, while 5% to 20% of symptomatic patients still reported these symptoms two years after infection. Far from being trivial, these chronic conditions can therefore represent a very heavy societal burden, both in terms of public health and the economy…
A few isolated cases of ocular, neurological (encephalitis, Guillain-Barré syndrome), and cardiac (myocarditis) complications have also been reported.
Fortunately, deaths from chikungunya are rare (between 0.1 and 1 per 1,000 symptomatic cases). They mainly affect newborns, for whom the disease is very dangerous, causing neurological and cardiac problems, as well as older adults or those with underlying health conditions (as the virus exacerbates these conditions).
Following exposure to the virus, our bodies develop long-lasting immunity that generally persists for several years, or even decades. In many cases, this protection may even last a lifetime. Reported cases of reinfection are very rare, suggesting that this acquired immunity is sufficient to protect most people exposed to the virus.
Diagnosis and Treatment
Because the symptoms are very similar to those of other viruses, such as the dengue virus or the Zika virus, it can be difficult to make a diagnosis.
The virus can be detected in blood samples using RT-PCR during the first week of the illness. Later on (after the fifth day), the infection can also be confirmed by testing for antibodies against the virus.
There is no antiviral medication for the chikungunya virus. Treatment focuses on relieving symptoms by administering pain relievers and fever reducers, such as acetaminophen, to manage pain and fever, as well as anti-inflammatory drugs to treat joint pain.
Since June 2024, a vaccine against chikungunya—the Ixchiq vaccine developed by Valneva—has been authorized for marketing in the European Union. It is a live attenuated vaccine: it contains a strain of the chikungunya virus that has been weakened in the laboratory and therefore can no longer cause the disease, but can stimulate the immune system.
Implemented during the major outbreak that affected Réunion in 2025, vaccination was suspended for individuals aged 65 and older, regardless of whether they had underlying health conditions. This was because several cases of serious adverse reactions had been reported in this age group. Further investigations are underway to assess the risk-benefit balance in older adults and adjust vaccination recommendations accordingly.
Epidemiology
The chikungunya virus has been circulating for several decades in Africa, India, and Asia, as well as in the Indian Ocean. In fact, it was the epidemic that struck Réunion, as well as Mauritius, Mayotte, and the Seychelles, in 2005–2006—affecting 38.2% of Réunion’s population—that helped bring it to the attention of the French public.
Before this first major outbreak, Réunion was not an area where the chikungunya virus circulated, because Aedes aegypti, the primary mosquito vector for this virus, is not established there. The tiger mosquito, Aedes albopictus, was present on the island, but was not known to transmit the virus. It was later discovered that a mutation had allowed the virus to adapt to this mosquito, which became a new vector. Now, several strains of the chikungunya virus circulate, depending on whether they are adapted to Aedes aegypti or the tiger mosquito. Since this change, the virus’s range has shifted considerably.
According to the World Health Organization (WHO), since 2004, chikungunya outbreaks have been reported in more than 110 countries in Asia, Africa, Europe, and the Americas. These outbreaks have become more frequent and widespread as populationsof Aedes aegypti andAedes albopictus have expanded.
In addition, adaptations that allow the virus to be transmitted more easily by the tiger mosquito have been detected. The fact that the virus was introduced into populations that had never been exposed to it (immunologically naive) also explains the increased frequency of outbreaks.
The Situation in France
In France, the risk of chikungunya virus transmission applies both to regions where Aedes aegypti is established, such as the French West Indies (Guadeloupe, Martinique, Saint Martin, Saint Barthélemy) and French Guiana, and to those where the Asian tiger mosquito (Aedes albopictus) is present, such as Réunion and mainland France. In Mayotte, which is home to both species of mosquitoes, the risk is high, particularly due to a favorable humid tropical climate.
It is estimated that approximately 80% of French departments meet the conditions conducive to the emergence of the disease, particularly due to the continued spread of the tiger mosquito throughout France. This mosquito is well established there: as of January 2024, it was present in 78 of the country’s 96 departments, not only in the south, but also in the Île-de-France region and as far east as the eastern part of the country.
Local cases of chikungunya—linked to infections occurring within the country rather than to travelers who were already infected upon arrival—have been reported in the past in mainland France. The very first local case of chikungunya in mainland France was identified in Fréjus, in the Var department, in September 2010. Since then, several sporadic outbreaks have been reported, mainly in southern France, including an outbreak of 11 cases in Montpellier (Hérault) in 2014 and 17 cases in the Var department in 2017.
The chikungunya virus had since become less prevalent, but in 2024, the first locally transmitted case was detected in the Île-de-France region, where the tiger mosquito has become established in recent years. The year 2025 is shaping up to be a record-breaking year, driven by the virus’s widespread circulation in Réunion and then in Mayotte: by early July, some thirty locally transmitted cases had already been detected in mainland France.
Steps to Take to Prevent Illness
At present, the only way to combat the disease is to protect oneself from bites and to control the mosquitoes that spread it.
To avoid getting bitten, wear light-colored, loose-fitting, and long-sleeved clothing (which reduces visual and thermal attractiveness to mosquitoes), use skin repellents, and set up mosquito nets (around your bed, on your windows, etc.).
To reduce the breeding of mosquito larvae, it is recommended that you empty all containers holding standing water—including flowerpot saucers and watering cans—and cover rainwater collection containers, especially during periods of heavy rainfall.
When a case of infection is reported, mosquito control operations are carried out in the vicinity of the detected cases, accompanied by public awareness campaigns targeting both the general public and healthcare professionals (through collaboration between regional health agencies, Santé publique France, and mosquito control agencies such as Altopictus orthe Interdepartmental Mosquito Control Association).
Tests to control populations of mosquito vectors using techniques such as the sterile insect technique are also underway.
Yannick Simonin, virologist specializing in the surveillance and study of emerging viral diseases. University Professor, University of Montpellier
This article is republished from The Conversation under a Creative Commons license. Readthe original article.